Table of Contents
Home pets get the best care, as they are constantly under the supervision of their owners. But they are not protected from various diseases. The Meloxicam oral suspension for dogs is known among veterinaries as an effective and affordable option for treating arthritis and pain.
What Is Meloxicam Oral Suspension?
It belongs to a group of non-steroidal medications that cause anti-inflammatory effects on the body. Also, it is prescribed for anesthesia and antipyretic, but a veterinarian’s consultation is necessary before the first use.
This medicine treats various musculoskeletal diseases in dogs, both active and chronic.
It is an FDA-approved non-steroidal, anti-inflammatory prescription medication (NSAID) used to help pets with degenerative or inflammatory joint conditions, such as osteoarthritis, rheumatoid arthritis, or juvenile rheumatoid arthritis. It helps alleviate pain, allowing your pet to live a happier and healthier life. In addition, NSAIDs improve your dog’s overall mobility by relieving joint pain and inflammation. This medicine may be used for other purposes; ask your veterinarian if you have questions.
Repeated medication use in cats has been associated with acute renal failure and death. Therefore, do not administer injectable or oral medication to cats without talking to your veterinarian.
It is available in the following forms:
- Oral liquid, 1.5 mg/mL (equivalent to 0.05 mg per drop) and 0.5 mg/mL (equivalent to 0.02 mg per drop). Oral Suspension 0.5 mg/mL: 15 mL and 30 mL dropper bottles with measuring syringe. Oral Suspension 1.5 mg/mL: 10, 32, 100, and 180 mL dropper bottles with measuring syringe. You can easily give oral suspension to your pet using the syringe that comes with the medicine. Best of all, you can even disguise it in your pet’s favorite wet food. Before giving the oral liquid, shake the bottle well. Carefully measure the dose as directed by your veterinarian.
- Oral spray (available in some countries only) is sprayed inside the cheek space.
- Injection (5 mg/mL solution for injection) is approved for a single injection to control pain associated with surgery in cats and dogs. Injectable forms for dogs and cats are available for veterinarian use only.
- It is also available in pill form, per 7.5mg.
Tablets and oral liquid can be given with or without food, but your dog should have access to clean water throughout the day. Give the medicine with food to reduce gastrointestinal side effects. Depending on the animal’s size, the drug can be given either on top of food or directly into the mouth.
Your veterinarian will provide you with specific instructions for administering the medication.
This medication will take effect quickly, in about 1 to 2 hours, and clinical signs should be improved.
Clinical Pharmacology
It is a non-steroidal anti-inflammatory drug (NSAID) of the oxicam class. The chemical name is 4-Hydroxy-2-methyl-N-(5-methyl-2-thiazolyl)-2H-1,2- benzothiazine-3-carboxamide-1, 1-dioxide. The formulation is a yellowish viscous suspension with the odor of honey.
It has nearly 100% bioavailability when administered orally with food. The terminal elimination half-life after a single dose is estimated to be approximately 24 hrs (+/-30%) regardless of the route of administration. There is no evidence of statistically significant gender differences in drug pharmacokinetics. Drug bioavailability, the volume of distribution, and total systemic clearance remain constant, up to 5 times the recommended dose for use in dogs. However, there is evidence of enhanced drug accumulation and terminal elimination half-life prolongation when dogs are dosed for 45 days or longer. Peak drug concentrations can occur within about 7.5 hours after oral administration. The corresponding peak concentration is approximately 0.464 mcg/mL following a 0.2 mg/kg oral dose. The drug is 97% bound to canine plasma proteins.
Effectiveness
Two field studies, including 277 dogs of various breeds, aged between six months and sixteen years, all suffering from osteoarthritis, showed that the drug was effective. Both of the 14-day, masked, placebo-controlled experiments were carried out. On the first day, 0.2 mg/kg of medicine was given to each dog. In addition, from days 2 through 14 of all investigations, all dogs were kept on 0.1 mg/kg of oral Meloxicam. Veterinarians assessed lameness, weight-bearing, palpable pain, and general progress. In addition, owners evaluated the following parameters: mobility, capacity to stand up straight, limping, and overall improvement.
The initial field research had 109 dogs, and after 14 days of meloxicam treatment, all metrics revealed clinically significant improvements in the canines.
In the second field study (48 dogs), dogs receiving the drug showed a clinical improvement after 14 days of therapy for all parameters; however, statistical significance was demonstrated only for the overall investigator evaluation on day 7 and the owner evaluation on day 14.
Safety
In a six-week target animal safety study, the medicine was administered orally at 1, 3, and 5x the recommended dose with no significant clinical adverse reactions. Animals in all dose groups (control, 1, 3, and 5x the recommended dose) exhibited some gastrointestinal distress (diarrhea and vomiting). Hematological, blood chemistry, urinalysis, clotting time, and buccal mucosal bleeding times showed no treatment-related alterations. Necropsy findings showed stomach mucosal petechiae in one control dog, two dogs given the 3x dose, and one dog given the 5x dose, and all had stomach mucosal petechiae. Other macroscopic alterations in three dogs at the 1x dose and two dogs at the 5x dose included regions of congestion or depression of the mucosa of the jejunum or ileum. Two canines in the control group displayed comparable alterations as well. With the 3x dose, no macroscopic small intestine lesions were seen in the dogs. Renal hypertrophy was noted during the necropsy of two dogs receiving the 3x dose and two dogs receiving the 5x dose.
Three dogs at the 5x dose showed minor degeneration or slight necrosis at the tip of the papilla upon microscopic inspection of the kidneys. Microscopic analysis of the stomach in two dogs at the approved dose, three dogs at the 3x dose, and four dogs at the 5x dose revealed inflammatory mucosal lesions, epithelial regenerative hyperplasia or atrophy, and submucosal gland inflammation. Small intestinal microscopic changes included minimal focal mucosal erosion affecting the villi and were sometimes associated with mucosal congestion. These lesions were observed in the ileum of one control dog, the jejunum of one dog at the recommended dose, and two dogs at the 5X dose.
In a six-month target animal safety study, the drug was administered orally at 1, 3, and 5x the recommended dose with no significant clinical adverse reactions. However, all animals in all dose groups (controls, 1, 3, and 5x the recommended dose) exhibited some gastrointestinal distress (diarrhea and vomiting). Treatment-related changes seen in hematology and chemistry included:
- decreased red blood cell counts in seven of 24 dogs (four 3x and three 5x dogs);
- decreased hematocrit in 18 of 24 dogs (including three control dogs);
- dose-related neutrophilia in one 1x, two 3x, and three 5x dogs;
- evidence of regenerative anemia in two 3x and one 5x dogs.
An increased BUN in two 5x dogs and decreased albumin in one 5x dog was also noted. Endoscopic changes included reddening the gastric mucosal surface covering less than 25% of the surface area. This was seen in three dogs at the recommended dose, three at the 3x dose, and two at the 5x dose. Two control dogs exhibited reddening with ulceration of the mucosa covering less than 25% of the surface area. Gross gastrointestinal necropsy results observed included mild discoloration of the stomach or duodenum in one dog at the 3x and another at the 5x dose. Multifocal pinpoint red foci were observed in the gastric fundic mucosa in one dog at the recommended dose and in one dog at the 5x dose.
This six-month study observed no macroscopic or microscopic renal changes in dogs receiving the medication. Microscopic gastrointestinal findings were limited to one dog at the recommended dose and two dogs at the 3x dose. A mild inflammatory mucosal infiltrate was observed in the duodenum of one dog at the recommended dose. In addition, mild congestion of the fundic mucosa and mild myositis of the outer mural musculature of the stomach were observed in two dogs receiving the 3x dose.
Ingredients
The drug has a balanced composition and begins to work after the first application. The main ingredient helps significantly reduce leukocyte infiltration into infected tissue.
Each ml of the suspension for dogs consists of the following:
- Meloxicam BP – 1.5 mg;
- Excipients – q.s.
Usage
Before using the drug, study the instructions and find out the dosage. Medication should only be used after consultation with the veterinarian.
Dosage forms
The oral suspension has two separate strengths, 0.5 mg/mL and 1.5 mg/mL. Don’t switch between them, as one is three times more concentrated than the other. Always use the correct oral syringe or dropper that comes with the medication.
Dosage for Dogs
A veterinarian can determine the ideal dosage of liquid medication for dogs. However, the dosage varies based on the condition in general.
The suggested dosage for osteoarthritis treatment is 7.5 mg once daily.
The oral dose is the same for dogs suffering from rheumatoid arthritis.
The recommended dosage for treating juvenile rheumatoid arthritis ranges from 0.125 mg/kg to 7.5 mg once daily.
Recommended Dosage
Your veterinarian carefully considers the benefits and risks of oral suspension and other treatment options before prescribing the medicine. Use the lowest effective dose for the shortest duration consistent with individual response.
The drug should be administered initially at 0.09 mg/lb (0.2 mg/kg) body weight only on the first day of treatment. All treatments after day 1 should be administered once daily at a dose of 0.045 mg/lb (0.1 mg/kg). The syringe is calibrated to deliver the daily maintenance dose in pounds.
Please take note: Use the Client Information Sheet to determine how to prepare the dose (syringe or dropper) and give the dose based on your dog’s weight and the medication’s dose concentration (directly into the mouth or mixed in with the food).
Before using the drug, carefully weigh the advantages and disadvantages of this medication and other available therapeutic choices. Then, use the shortest possible duration at the lowest effective dose following individual reaction.
Directions for administration of 1.5 mg/mL strength
Dogs under 10 pounds (4.5 kg)
Shake well before use, then remove the cap. Regarding dosage accuracy, extra attention should be used. Give drops only on food to little dogs – never directly into their mouths – to prevent unintentional overdoses. Before giving the dog the food, carefully measure the suspension onto it to ensure the right dose is given. The syringe in the drug with a concentration of 1.5 mg/mL cannot be used to measure doses for dogs weighing less than 5 lbs (2.3 kg).
For dogs under 5 lbs (2.3 kg), the drug can be given using the dropper bottle: one drop for each pound of body weight for the 1.5 mg/mL concentration (two drops for each kilogram), dropped directly onto the food.
Dogs between 5-10 pounds can be given by drops or using the measuring syringe provided in the package. The syringe fits onto the bottle and has a scale beginning at 5 lbs, designed to deliver the daily maintenance dose (0.05 mg/lb or 0.1 mg/kg). The dog’s weight should be rounded to the nearest 5-pound increment when using the syringe. Replace and tighten the cap after use.
Dogs over 10 pounds (4.5 kg)
Shake well before use, then remove the cap. The drug may be mixed with food or placed directly into the mouth. Particular care should be given concerning the accuracy of dosing. It can be given using the measuring syringe provided in the package. The syringe fits onto the bottle and has a pound scale designed to deliver the daily maintenance dose (0.05 mg/lb or 0.1 mg/kg). The dog’s weight should be rounded to the nearest 5-pound increment when using the syringe. Alternatively, the drug can be given using the dropper bottle: one drop for each pound of body weight for the 1.5 mg/mL concentration (two drops for each kilogram). Replace and tighten the cap after use.
Directions for administration 0.5 mg/mL strength
Dogs under 10 pounds (4.5 kg)
Shake well before use, then remove the cap. Regarding dosage accuracy, extra attention should be used. Give drops only on food to little dogs – never directly into their mouths – to prevent unintentional overdoses. Before giving the dog the food, carefully measure the suspension onto it to ensure the right dose is given. The syringe with a 0.5 mg/mL concentration cannot be used to measure doses for dogs weighing less than 1 lb (0.45 kg).
The drug can be given using the dropper bottle for dogs less than 1 lb (0.45 kg): two drops for each pound of body weight for the 0.5 mg/mL concentration (five drops for each kilogram), dropped directly onto the food.
For dogs between 1-10 pounds, the medicine can be given by drops or using the measuring syringe provided in the package (see dosing procedure below). The syringe fits onto the bottle and has a scale beginning at 1 lb, designed to deliver the daily maintenance dose (0.05 mg/lb or 0.1 mg/kg). The dog’s weight should be rounded to the nearest 1-pound increment when using the syringe. Replace and tighten the cap after use.
Dogs over 10 pounds (4.5 kg)
Shake well before use, then remove the cap. The drug may be mixed with food or placed directly into the mouth. Particular care should be given concerning the accuracy of dosing. The medicine can be given using the measuring syringe provided in the package. The syringe fits onto the bottle and has a pound scale designed to deliver the daily maintenance dose (0.05 mg/lb or 0.1 mg/kg). The dog’s weight should be rounded to the nearest 1-pound increment when using the syringe. Alternatively, the liquid can be given using the dropper bottle: two drops for each pound of body weight for the 0.5 mg/mL concentration (five drops for each kilogram). Replace and tighten the cap after use.
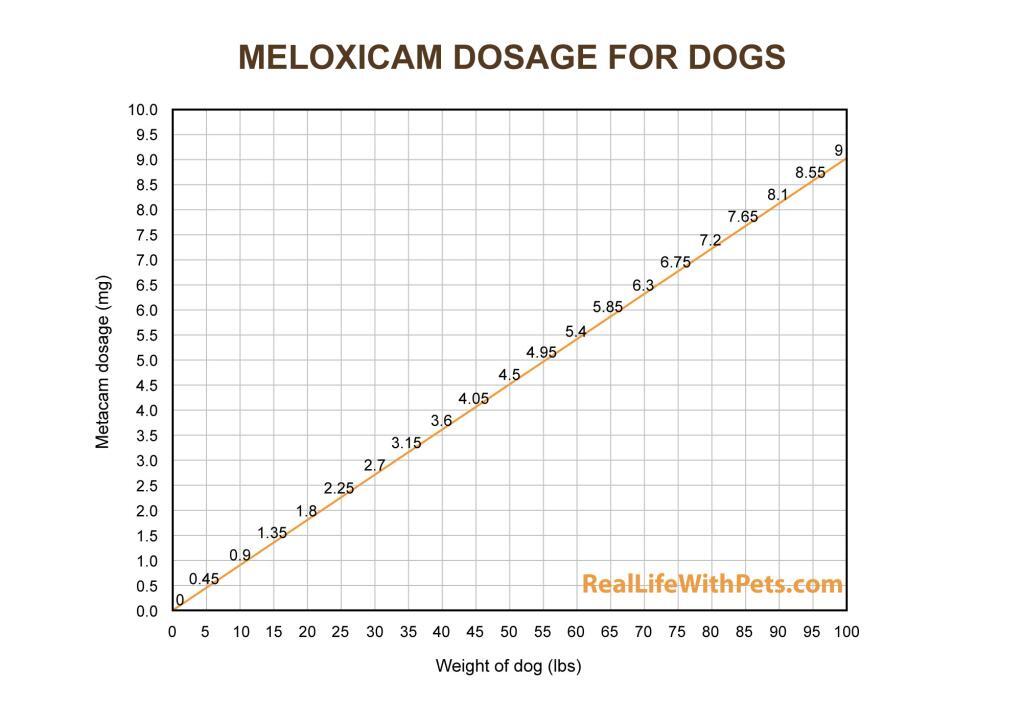
Method of Administration
The suspension is injected into the body of dogs using a dropper bottle. The dose is calculated according to the weight of the animal.
Take this medicine orally. Follow the directions on the prescription label. Shake well before using. Use a specially marked spoon or dropper to measure each dose. Ask your pharmacist if you do not have one. Household spoons are not accurate.
You can give it with or without food. If it upsets the stomach, give it with food. Give the medicine at regular intervals. Please do not give it more often than directed. Do not stop giving except on your vet’s advice.
Talk to your veterinarian regarding the use of this medicine in puppies.
| How Long Will a Bottle Last My Dog? | ||||
| Dog’s Size (kg) | Bottle Size | |||
| 10 ml | 32 ml | 100ml | 180 ml | |
| Period of Treatment | ||||
| Approx.Number of Days | Approx.Number of Days | Approx.Number of Weeks | Approx.Number of Weeks | |
| 5 | 30 | 96 | n/a | n/a |
| 10 | 15 | 48 | 21 | n/a |
| 15 | 10 | 32 | 14 | n/a |
| 20 | 7 | 24 | 11 | 19 |
| 25 | 6 | 19 | 9 | 15 |
| 30 | 5 | 16 | 7 | 13 |
| 35 | 4 | 13 | 6 | 11 |
| 40 | 3 | 12 | 5 | 10 |
| 45 | 3 | 10 | 5 | 8 |
What if I Miss Giving My Pet a Dose?
If you forget to give your pet a dose, give the subsequent dose as soon as you remember. However, if the interval between the missing dose and the subsequent one is less than 12 hours, skip the missed dose and provide the subsequent one instead. Or administer the missed dose and then wait the advised time before administering the subsequent dose (continue giving it regularly at that new time).
Give your pet only one dose at a time. Never give an extra dose.
Withdrawal Time
The time of complete withdrawal of the drug from the animal’s body depends on the duration of its use, as well as the weight of the dog. In actual terms, there are no withdrawal symptoms associated with the drug. But it takes the body between 15 and 20 hours to metabolize and expel half the drug out of the system.
On average, withdrawal time is 5 to 7 days from the end of long-term therapy. Do not give other NSAID drugs (e.g., carprofen, deracoxib) or glucocorticoids (e.g., prednisone, dexamethasone) 5-7 days after stopping this medication or until your veterinarian tells you to start.
Important Safety Information for Dog Owners
The owner should learn some essential points before starting to succeed during therapy with this liquid for dogs. Thus, all possible risks will be reduced to zero.
Warning: Repeated use in cats has been associated with acute renal failure and death. Do not administer injectable or oral drugs to cats unless your veterinarian prescribes them. See Contraindications, Warnings, and Precautions for detailed information.
Before giving this medicine to your dog, tell your veterinarian if your dog has or had the following conditions:
- bleeding disorders;
- coronary artery bypass graft (CABG) surgery within the past two weeks;
- heart disease;
- history of stomach bleeding;
- kidney disease;
- liver disease;
- lung or breathing disease;
- stomach or intestine problems;
- an unusual or allergic reaction to the medicine, aspirin, other NSAIDs, other medicines, foods, dyes, or preservatives;
- pregnant;
- nursing.
Owners should be aware of the possibility of negative responses and the clinical symptoms linked to drug intolerance. Vomiting, diarrhea, decreased appetite, dark or tarry stools, increased water intake, increased urination, pale gums due to anemia, yellowing of the gums, skin, or whites of the eyes due to jaundice, lethargy, incoordination, seizure, or behavioral changes are just a few examples of adverse reactions. This medicine class’s severe side effects occasionally cause fatalities and can happen without warning (see Side Effects). Therefore, owners should be advised to discontinue treatment and contact their veterinarian immediately if intolerance is observed.
Most patients with drug-related adverse reactions have recovered when the signs are recognized, the drug is withdrawn, and veterinary care, if appropriate, is initiated. However, owners should be advised of periodic follow-ups for all dogs while administering any NSAID.
Other drugs can interact with this drug. Be sure to tell your veterinarian and pharmacist what medications (including vitamins, supplements, or herbal therapies) you give your animal, including the amount and time you give each. In addition, tell your veterinarian about any conditions or diseases your animal may have now or has had in the past.
If your animal has been treated for the same disease or condition, tell your veterinarian about the treatment and how well it did or didn’t work.
If your animal is pregnant or nursing, talk to your veterinarian about the drug’s risks. Also, tell your veterinarian and pharmacist about any medication side effects (including allergic reactions, lack of appetite, diarrhea, itching, and hair loss) your animal has developed in the past.
Palatability
The drug was accepted by 100% of the dogs when veterinarians administered the initial dose into the mouth. The drug was accepted by 90% of the dogs (123/136) when administered by owners. Problems associated with administration included refusal of food, resistance to swallowing, and salivation.
Veterinary Prescription
It is a strong painkiller and needs to be prescribed by a veterinarian. According to federal law, this medication can only be used by or on the advice of a licensed veterinarian.
The drug is an FDA-approved non-steroidal anti-inflammatory drug (NSAID) available as a prescription medication to reduce pain, inflammation, and fevers in dogs.
Your veterinarian may recommend blood testing before and after using the drug to monitor liver and kidney function or to detect other signs consistent with gastrointestinal ulceration. In addition, it is common for your veterinarian to recommend or require annual blood tests to assess for effects on organ function.
Contraindications and Warnings
No drug is 100% safe for all patients, but your veterinarian will discuss any specific concerns about using this drug. The medication should not be used in patients with allergies to aspirin or other NSAIDs.
It should not be used in:
- pets with bloody stools or vomit;
- pets that have pre-existing kidney or liver conditions;
- pets that have a loss of appetite;
- pets that are taking other NSAIDs (e.g., carprofen, etodolac, firocoxib, and aspirin) or corticosteroids (e.g., prednisone and dexamethasone);
- dehydrated pets;
- breeding, pregnant, and lactating animals;
- puppies younger than six months or kittens under four months of age.
The drug should be used with caution on the following pets:
- cats (see above);
- pets that have ulcers or have had them in the past;
- pets that have pre-existing heart conditions;
- pets that are old, weak, or frail;
- pets on diuretic treatment(e.g., furosemide, hydrochlorothiazide);
- pets that have a bleeding disorder.
It is not known if the medicine is safe to use on these animals:
- Pets with a bleeding disorder (e.g., von Willebrand disease).
- Old, weak pets.
If your animal has any of these conditions, talk to your veterinarian about the potential risks versus benefits.
Interactions
Do not take this medicine with any of the following medications:
- cidofovir;
- ketorolac.
This medicine may also interact with the following medications:
- aspirin and aspirin-like medicines;
- some drugs to treat or prevent blood clots, such as warfarin, enoxaparin, dalteparin, apixaban, dabigatran, and rivaroxaban;
- certain drugs to treat or prevent high blood pressure, heart disease, and irregular heartbeat;
- certain medicines for depression, anxiety, or psychotic disturbances;
- cyclosporine;
- diuretics;
- fluconazole;
- lithium;
- methotrexate;
- other NSAIDs, medicines for pain and inflammation, like ibuprofen and naproxen;
- pemetrexed.
This list may not describe all possible interactions. Give your veterinarian a list of all the medicines, herbs, non-prescription drugs, or dietary supplements you give your pet.
Sensitivity to drug-associated adverse events varies with the individual patient. Dogs that have experienced adverse reactions from one NSAID may experience adverse reactions from another NSAID. Patients at greatest risk for renal toxicity are those dehydrated, on concomitant diuretic therapy, or those with existing renal, cardiovascular, and/or hepatic dysfunction.
NSAIDs may prevent prostaglandins from maintaining healthy homeostasis. Patients with undiagnosed underlying or pre-existing diseases may experience clinically substantial disease due to anti-prostaglandin effects. Combining NSAIDs with corticosteroids or other anti-inflammatory medications should be avoided because they both have the potential to cause gastrointestinal ulcerations and/or perforations. If additional pain medication is needed after administration of the total daily dose of this drug, a non-NSAID or non-corticosteroid class of analgesia should be considered. The use of another NSAID is not recommended. Consider appropriate washout times when switching from corticosteroid use or one NSAID to another in dogs. The use of concomitantly protein-bound drugs with this medication has not been studied in dogs. Commonly used protein-bound drugs include cardiac, anticonvulsant, and behavioral medications. The influence of concomitant drugs that may inhibit the metabolism of this drug has not been evaluated. Drug compatibility should be monitored in patients requiring adjunctive therapy.
Caution must be taken when this drug is used in conjunction with many different drugs, including the following:
- antibiotics (e.g., gentamicin, amikacin);
- anesthetics, anticoagulants (e.g., heparin, warfarin);
- diuretics (e.g., furosemide);
- antifungals (e.g., fluconazole);
- immunosuppressive (e.g., methotrexate, cyclosporine);
- corticosteroids (such as prednisone and prednisolone);
- other NSAID drugs.
Precautions
This medication is for oral use in dogs only. Do not administer it to cats. See Contraindications, Warnings, and Precautions for detailed information.
As a class, cyclo-oxygenase inhibitory NSAIDs may be associated with gastrointestinal, renal, and hepatic toxicity. The most common side effects are vomiting and soft stool or diarrhea. These are usually mild and affect the gastrointestinal system primarily, but more severe side effects can occur. Therefore, NSAIDs should only be administered under the direction of a licensed professional. If you notice side effects in your dog during treatment, stop the drug and call your veterinarian. Dogs should be evaluated for pre-existing conditions and currently prescribed medications before treatment, then monitored regularly while on therapy. Concurrent use with another NSAID, corticosteroid, or nephrotoxic medication should be avoided or monitored closely.
Not for use in humans. Keep this and all medications out of reach of children. Consult a physician in case of accidental ingestion by humans. Dogs with known hypersensitivity to Meloxicam should not receive it.
The medicine can be used in the treatment of dog infections only orally. Therefore, before starting therapy, a sick dog should be well-observed. For dogs that are hypersensitive to the medication, the use of oral suspension is unacceptable.
During the entire period of therapy, it is recommended to conduct appropriate laboratory tests to establish the initial hematological and biochemical parameters of blood serum. In addition, the owner should monitor the pet to identify possible signs of the drug’s potential toxicity.
Call your veterinary office immediately if you suspect an overdose or an adverse reaction to the medication. If they are unavailable, follow their directions to contact an emergency facility.
Side Effects
The drug is not free from adverse reactions like other drugs. Therefore, owners who buy it should be warned about possible adverse reactions. The drug is tolerated well in most animals, but rare, serious side effects (e.g., stomach ulcers, liver or kidney problems) and sometimes death have been reported.
Meloxicam side effets:
- Gastrointestinal reactions to the drug: vomiting, diarrhea, partial or complete loss of appetite, melena, hemorrhage.
- Nervous damage: ataxia, convulsions, drowsiness, hyperactivity, depression, trembling.
- Kidney problems: increased creatinine levels, as well as symptoms of acute renal failure.
- Skin reactions: itching, eczema, focal alopecia, wet dermatitis (hot spots), pruritus.
- Hypersensitivity: urticaria, allergic dermatitis.
- Problems with the circulatory system: hemolytic anemia, thrombocytopenia.
- Liver: Increased levels of liver enzymes, jaundice.
- Urinary: azotemia, elevated creatinine, renal failure.
- Neurological/Behavioral: lethargy, depression.
- Hepatic: elevated liver enzymes.
Additional Information About Side Effects
The safe use of the drug in dogs younger than six months of age, dogs used for breeding, or pregnant or lactating dogs has not been evaluated. With your veterinarian, carefully consider the potential benefits and risks of the drug and other treatment options before deciding to use Meloxicam.
Use the lowest effective dose for the shortest duration consistent with individual response.
Field safety was evaluated in 306 dogs. Based on the results of two studies, GI abnormalities (vomiting, soft stools, diarrhea, and inappetence) were the most common adverse reactions associated with administering the drug. The following table lists adverse reactions and the number of dogs that experienced them during the studies. Dogs may have experienced more than one episode of the adverse reaction during the study.
| Side Effects Observed During Two Field Studies | ||
| Clinical Observation | Meloxicam (n=157) | Placebo (n=149) |
| Vomiting | 40 | 23 |
| Soft Stool/Diarrhea | 19 | 11 |
| Bloody Stool | 1 | 0 |
| Inappetance | 5 | 1 |
| Swollen Carpus/Lethargy | 1 | 0 |
| Bleeding gums after dental procedure | 1 | 0 |
| Epiphoria | 1 | 0 |
In foreign suspected adverse drug reaction (SADR) reporting over nine years, incidences of adverse reactions related to the medicine administration included:
- auto-immune hemolytic anemia (1 dog);
- thrombocytopenia (1 dog);
- polyarthritis (1 dog);
- nursing puppy lethargy (1 dog);
- pyoderma (1 dog).
Post-Approval Experience (Rev. 2010): The following adverse events are based on post-approval adverse drug experience reporting. Not all adverse reactions are reported to FDA/CVM. Therefore, using these data, estimating the adverse event frequency or establishing a causal relationship to product exposure is not always possible. The following adverse events are listed in decreasing frequency by the body system.
Death has been reported as an outcome of the adverse events listed above. In addition, acute renal failure and death have been associated with using this drug in cats.
Dogs: The most common side effect in dogs is gastrointestinal upset, including vomiting, soft stools, and lack of appetite.
Rarely severe adverse effects can occur. For example, if there are changes in urination or yellowing of the skin (often noted on the inside of ear flaps), stop giving the medication and contact your veterinarian immediately.
Cats: It should be used with caution in cats. Cats with early undiagnosed kidney disease can suffer kidney damage, depending on the dose prescribed. Therefore, your veterinarian will carefully weigh the pros and cons of medicating your cat with this medication and may order blood work and urinalysis to check your cat’s kidney function before prescribing the drug. In addition, gastrointestinal upset, including vomiting, diarrhea, and lack of appetite, are sometimes side effects in cats.
Never give the drug prescribed for one pet in your household to another without consulting your veterinarian.
Any side effects that you observe should be reported to your veterinarian.
This moderate-acting medication should stop working in a few days, although the effects can be longer in pets with liver or kidney disease.
Overdose
If your puppy begins to show symptoms such as nausea, vomiting, loss of appetite, or weight loss during treatment with this drug, immediately stop therapy and consult a veterinarian.
Poisoning
Meloxicam for dogs is known by the brand name Metacam. The drug has few side effects in the recommended dose and will likely help your dog with pain. However, high doses can cause kidney failure and stomach ulcerations, so giving your dog the prescribed amount is crucial to avoid overdose. In dogs, it is given orally or via injection.
In clinical trials, dogs could take this 0.1 mg per kg dose safely for 26 weeks with no adverse side effects; however, signs of toxicity developed with higher doses of 0.3-0.5 mg per kg.
Meloxicam poisoning is typical of other NSAID’s with vomiting and diarrhea being the most common adverse reactions. Vomit and stool may contain signs of blood from gastrointestinal ulceration. GI signs are often combined with symptoms of kidney failure – increased urination and thirst. Dogs will lose their appetite and may seem generally weak and depressed. Overdose can cause severe gastrointestinal bleeding, seizures, and fatal kidney failure.
Symptoms of Meloxicam Poisoning in Dogs
These are the signs you may see in a dog with toxicity. Contact a veterinarian immediately if an overdose is suspected.
- Vomiting (with or without blood);
- diarrhea (sometimes with blood);
- lack of appetite;
- black tarry stools (melena);
- excessive thirst (polydipsia);
- frequent urination (polyuria);
- lethargy;
- general malaise;
- abdominal pain;
- seizures.
Causes of Poisoning in Dogs
These are dogs’ most common causes and risk factors for Meloxicam toxicity:
- giving your dog doses more frequently than was prescribed;
- accidental overdose (container was left open, dog chewed through the bottle);
- giving a dog medication intended for humans.
Diagnosis of Poisoning in Dogs
The veterinarian will diagnose poisoning in your dog based on symptoms, a history of Meloxicam use, and blood tests or urinalysis. Diarrhea, vomiting, and bloody stools may suggest the dose is too high or your dog is not tolerating the medication well. Depending on the severity, lab work will show an increased BUN (blood urea nitrogen) and other changes indicative of kidney failure.
Bring the prescription along so the veterinarian can see the exact dosage, and let the veterinarian know if there is any chance your dog accidentally overdosed or was given extra. Any other medications your dog takes are also relevant since adverse reactions to other drugs can complicate poisoning. The veterinarian must also know if your dog can reach human medication. It’s a good idea to bring a list of the drugs you or other household members are taking, especially if you didn’t see the incident and are unsure what is causing your dog’s signs.
Treatment of Meloxicam Poisoning in Dogs
If your dog is showing signs of toxicity, discontinuing the dose may be sufficient, depending on the severity of the signs. However, for significant overdose, other treatment will be necessary.
Vomiting may be induced a few hours after exposure. Activated charcoal may be given to reduce absorption in the gastrointestinal tract. This dose may be repeated in 6-8 hours to avoid recirculation from the liver. Cathartic medication can help induce bowel movements and excrete toxins faster.
Various medications may be given to treat gastrointestinal ulcers, including H2-receptor antagonists like ranitidine and famotidine or a proton pump inhibitor like Omeprazole. In addition, Sucralfate and misoprostol have been found to protect the stomach and reduce ulcer formation of ulcers, so these medications may also be prescribed.
If kidney failure is present, IV fluids will be necessary. In addition, your dog will need to stay at a veterinary hospital for monitoring for 72 hours or until the kidneys function normally.
Recovery of Poisoning in Dogs
The drug has been approved for dogs, but certain risks remain. The veterinarian should inform you of the side effects when the drug is prescribed so that you can watch your dog closely and treat any signs of toxicity as soon as possible. Taking the exact dose is extremely important. Cutting up a tablet or a generic medication designed for humans is not recommended since it is too hard to regulate the amount with this method, and you may be accidentally giving your dog a slight overdose. Even a fraction of a milligram can make a difference with this medication. If you forget to give your dog a dose, give it as soon as possible; however, if it is too close to the next medication time, it’s better to miss a dose than give two at once.
This drug toxicity can be fatal, so getting treatment immediately is important. The best way to manage the condition is to avoid exposure. Keep all bottles securely fastened and store them out of your dog’s reach. Coordinate medication with other household members to ensure your dog isn’t getting several doses by accident. Keep human and dog medication separate so there is no confusion.
Storage
This drug does not require special storage conditions. It is enough to keep it at a controlled room temperature, 68-77 F (20-25 C), away from direct sunlight.
Brief exposure to temperatures up to 104 F (40 C) may be tolerated, provided the mean kinetic temperature does not exceed 77 F (25 C); however, such exposure should be minimized.
Not for use in humans. Keep this and all medications out of reach of children and animals. For oral use in dogs only.
Benefits
- The drug has been used for over 20 years and has helped control osteoarthritis pain in dogs in over 30 countries.
- Syringe calibrated by body weight in pounds makes dosing convenient and precise.
- Dogs love the sweet, honey-flavored taste.
- Easily applied to the dog’s food or given directly into the dog’s mouth.
- Ease of use makes it ideal for improved client compliance.
- Individualized dosing ensures that each dog receives precisely what they need.
- It is a surprisingly good fit for a dog owner’s pocketbook in 2022.
- Titration to the lowest effective dose can help owners save even more.
Drugs Similar to Meloxicam
The most common brand names are Melonex Oral, Metacam, Loxicom, Meloxidyl, Inflacam, and Rheumocam.
Drugs similar to Meloxicam are:
- Carprofen (common brand names: Rimadyl, Carprieve, Rimifin, Carprox, Rycarfa)
- Robenacoxib (common brand name: Onsior).
FAQs
What Is the Best Anti-Inflammatory for Arthritis in Dogs?
Non-steroidal anti-inflammatory drugs (NSAIDs) play a significant role in controlling dog joint pain and inflammation. Prescription medication such as Meloxicam is the safest option for controlling pain and inflammation compared to over-the-counter, non-veterinary products.
Where to Purchase the Drug in 2023?
You can buy it in an online pharmacy store for pets. The price is affordable in 2023. By the way, the more you buy, the more you save.
How Much Does It Cost?
The cost depends on the form and dosage. In 2023 it will be available online at affordable prices with quick delivery directly to you.
Where Was That Drug Created?
It was created in India. The name of the manufacturer is Intas.
How Much Liquid Medication Can I Use to Treat My Dog?
The dose varies from 0.125 mg/kg to 7.5 mg once daily. Please read the dosage information or contact the vet for a more accurate dosage.
Can I Give My Dog 15 mg of the Drug?
The recommended dosage is around 0.09 milligrams per pound of your dog’s body weight on the first day. After the first treatment, all subsequent treatments should be given once a day. Your vet should prescribe the first and further dosage.
What Happens if I Give My Dog Too Much of the Drug?
NSAIDs can cause severe stomach ulcers and abrupt renal failure when consumed at hazardous doses. Toxic symptoms include nausea, vomiting, diarrhea, bloody vomitus, black-tarry stools, lack of appetite, passive behavior, excessive thirst or urination, general malaise, abdominal pain, seizures, or even death.
How Does It Work?
It targets and relieves both the pain and inflammation caused by osteoarthritis. Relief from arthritis pain can help restore mobility, allowing your dog to return to many activities you both previously enjoyed. Best of all, it can be given once daily, which provides 24 hours of relief.
What Else Can I Do to Help My Dog Overcome Pain?
Meloxicam therapy is one of many things that may help relieve your dog’s osteoarthritis pain. Your veterinarian may suggest a weight loss program or exercise regimen. Talk to your veterinarian before starting your dog on any weight loss or exercise plan. You can also help to make your dog as comfortable as possible by providing a quiet place to sleep and keeping them warm. Performing massage and physical therapy on your dog as directed by your veterinarian can relieve joint stiffness and increase the range of motion. In addition, raising food and water bowls to avoid neck strain, installing ramps to avoid your dog having to use stairs, putting non-skid runners on slippery surfaces, and other supportive measures can help make daily activities less painful.
What Should I Choose: Meloxicam Tablet or Liquid?
It depends on the disease’s course and your dog’s size and weight. The liquid form is better suited for the initial stages of treatment and is also more favorable for dogs with diseases of the gastrointestinal tract.
Why Is It Easier to Find Meloxicam Oral Liquid Rather Than a Pill?
Liquid is more popular because it is designed to make administering the correct dose to dogs easier. The oral suspension is made in a smooth liquid form so dog owners can dispense it easily from the syringe. Because it’s liquid, it is easy to adjust the dose using the measuring syringe in small increments, with a precision unavailable from a rigid tablet. It is easily applied to the dog’s food or given directly into the dog’s mouth. Moreover, liquid medication is readily absorbed by dogs. And dogs love the sweet honey-flavored taste.
Can the Drug Be Used in Very Small Dogs?
Small-breed dogs may also have osteoarthritis. That’s why a special low-concentration oral suspension for small dogs was developed.
How Long Should My Dog Take Meloxicam?
Your veterinarian will recommend a treatment plan and suggest your dog try the drug for a specific period. Your veterinarian may ask you to report or return with your dog for a follow-up evaluation to determine if treatment should continue. Just like people who have osteoarthritis, your dog will likely have to live with this condition for the rest of his life. You may feel comfortable giving the drug knowing it has been safely used to treat dogs with osteoarthritis worldwide for over 20 years.
How Long Until I know if This Medication Is Working, and How Long Will the Effects of This Medication Last?
This medication should help your animal feel better within 1 to 2 hours. Your animal’s clinical signs should improve after that time. The effects of this medication are moderate in duration, meaning they may last for a few days, although the benefits may be prolonged if your animal has decreased kidney and/or liver function.
How Effective is Meloxicam for Dogs?
Veterinarians most frequently prescribe it to treat dogs with osteoarthritis-related inflammation, discomfort, and stiffness. Still, it can also treat symptoms of other muscle or bone problems. This is because it functions by lowering the hormones that produce pain and inflammation in the body, and because it is an NSAID, it does so without using steroids.
How Does the Drug Make a Dog Feel?
When your dog starts treatment, you will likely notice an increase in your dog’s activity level. Once the spark is back, your dog may be more energetic, just like he used to be.
Can Handling This Medication Be Hazardous to Me, My Family, or Other Animals?
No specific precautions are required when handling this medication unless you are allergic to it. Wash your hands after handling any medication.
Does Meloxicam for Dogs Expire?
Like all medications, it has its expiry date on the package. Please do not use it after the expiration date.
Does Meloxicam for Dogs Need to Be Refrigerated?
Store the drug at room temperature.
How Should I Dispose of This Medication if I Don’t Use It All?
This drug should not be washed down the sink or flushed down the toilet. Instead, use the community drug “take-back” program if one is offered. If there is no take-back program, mix the medicine with coffee grounds or cat litter to disguise it from children, animals, and anyone looking through your trash. Then, put the mixture in a sealable plastic bag to prevent leakage, and throw the bag out with the regular trash.
Can I Use Human Meloxicam On My Dog?
While the drug may be administered directly into the mouth of a larger dog, it is often given indirectly to smaller dogs by putting it in their food. However, a large dog may technically take a portion of a Mobic tablet safely if your veterinarian recommends it. Unfortunately, getting an accurate dosage using human tablets is difficult for most dogs, so you should do it under your vet’s prescription.
Can I Give Meloxicam for Dogs to My Cat?
No. Although it is designed to relieve pain and inflammation in cats and dogs, the situations in which you use it are different for both. Repeated medication use in cats has been associated with acute renal failure and death. Therefore, do not administer injectable or oral medication to cats without talking to your veterinarian.
Can Meloxicam Kill a Dog?
This drug toxicity can be fatal, so getting treatment immediately is important. The best way to manage the condition is to avoid exposure. Keep all bottles securely closed and store them out of your dog’s reach.
How Long Can a Dog Stay on Meloxicam?
Your dog may stay on this medication as long as your vet considers it reasonable. But remember, as with all veterinary NSAIDs, periodic monitoring tests are important to check liver enzymes and kidney function and generally screen the patient’s health. Typically an every six months schedule is recommended for dogs.
Is It OK to Stop Taking Meloxicam Suddenly?
Because it does not affect the systems usually associated with addiction potential, it is considered a nonaddictive drug from that standpoint. As a result, stopping use is unlikely to cause withdrawal symptoms that present with addictive substances and can be stopped abruptly without risk.
Can I Cut Meloxicam in Half?
Tablets are light round yellow, flat, scored tablets embossed with AX5 on one side, which can be divided into equal halves. But remember that the dosage of pill medication is not precise. For small dogs, it can be very dangerous. Please get in touch with your vet to get dosage recommendations.
What Are the Dangers of Taking This Drug?
When using this medication, serious adverse effects are possible and can happen suddenly. You may notice probable warning signs, such as excruciating stomach pain, bloody or coffee-ground-looking vomiting, skin rash, and swelling of the face, fingers, feet, or lower legs.
Can the Drug Cause Kidney Failure in Dogs?
NSAIDs can cause severe stomach ulcers and abrupt renal failure when consumed at hazardous doses. Toxic symptoms include nausea, vomiting, diarrhea, bloody vomitus, black-tarry stools, lack of appetite, passive behavior, excessive thirst or urination, general malaise, abdominal pain, seizures, or even death.
Does Meloxicam Make Dogs Sleepy?
Excessing this drug in dogs may lead to overdose and even death. One of the possible side effects is excessive sedation.
Can the Drug Cause Seizures?
Call the poison control helpline if a dog has taken too much. Call the emergency center immediately if the dog has a seizure, has difficulty breathing, collapses, or cannot be woken up. It is a symptom of an overdose.
Does This Medication Cause Liver Damage in Dogs?
As a class, cyclo-oxygenase inhibitory NSAIDs may be associated with gastrointestinal, kidney, or liver side effects. Call your veterinarian if you notice any side effects.
Does It Cause Constipation in Dogs?
Its most common side effects involve digestive issues such as vomiting and decreased appetite. Other possible side effects include changing bowel movements (black, tarry, bloody stools, diarrhea).
Does Meloxicam Make Dogs Pant?
It is unlikely to be a side effect of the drug. It is pretty well tolerated in dogs without any common side effects, though occasionally vomiting is seen. Panting may be more commonly caused by obesity or joint pain from arthritis he probably has.
Does It Make Dogs Thirsty?
Yes, symptoms of the drug include black or bloody diarrhea, bloody vomit, and increased thirst.
Can the Drug Cause Stomach Bleeding?
It may cause bleeding in the stomach or bowels. This problem can happen without warning signs. It may be a sign of an overdose or a side effect.
Can It Cause Allergic Reaction?
Just as with humans, there is a risk that your dog may have an allergic reaction to a medication. Contact your vet immediately if you see any signs of an allergic reaction, like redness, swelling, or itchiness. The drug may cause a severe type of allergic reaction called anaphylaxis. Although rare, this may occur in patients allergic to aspirin or other non-steroidal anti-inflammatory drugs. Anaphylaxis can be life-threatening and requires immediate medical attention.
Does the Medication Cause Itching in Dogs?
Yes, skin irritation, redness, scabs, or scratching may occur. Please get in touch with your veterinarian if you notice any signs of side effects.
Will Side Effects Go Away and When?
Most common side effects are temporary and will decrease after the drug is discontinued. Unfortunately, the drug stays in the body much longer than other NSAIDs, so side effects may linger a day or two after the last dose.
What Are the Worst Side Effects?
Serious side effects can occur during treatment with this medicine and without warning. However, possible warning signs often occur, including severe stomach pain, black, tarry stools, vomiting of blood or material that looks like coffee grounds, skin rash, and swelling of the face, fingers, feet, or lower legs.
Can Dogs Have Human NSAIDs?
Over-the-counter (OTC) pain meds and other human medications can be dangerous and even fatal for dogs. Therefore, dogs should not be given ibuprofen (Advil), acetaminophen (Tylenol), aspirin, or any other pain reliever made for human consumption except under the direction of a veterinarian.
Can I Give My Dog Aspirin With Meloxicam?
This drug should not be given with any other NSAIDs, including Carprofen (Rimadyl), Firocoxib (Previcox), Etodolac (Etogesic), Deracoxib (Deramaxx), or Aspirin. In addition, please do not use it in dogs under six weeks of age or in pregnant, lactating, or breeding dogs, as it has not been evaluated.
Aspirin is a drug that is not approved for use in animals.
What Is the Difference Between Mobic and Metacam?
Mobic for humans is the generic equivalent of Metacam for dogs. Mobic is only meant for human consumption, while Metacam has been designed as a pain relief for dogs and cats.
Is Meloxidyl the Same as Meloxicam?
Studies have been carried out to prove that Meloxidyl is ‘bioequivalent’ to the reference veterinary medicinal product. This means that Meloxidyl is equivalent to this drug in how it is absorbed and used by the body. Meloxidyl is a liquid form of this medicine.
What Is the Difference Between Metacam and Lexicon?
The Lexicon contains the active ingredient Meloxicam and is a ‘generic medicine.’ This means that Loxicom contains the same active substance and works the same way as a ‘reference medicine’ already authorized in the European Union (EU) under the brand name Metacam.
Is Meloxicam the Same as Tramadol?
This drug and Tramadol are used to treat pain, so they are similar but not the same. They belong to different classes of drugs. This drug is an NSAID, and Tramadol is a narcotic painkiller. Both drugs may interact with alcohol, antidepressants, heart medication, or blood pressure medication.
Can a Dog Take Tramadol and Meloxicam Together?
Combining these two drugs resulted in an earlier decrease in postoperative pain scores than Tramadol alone or Tramadol with dipyrone. However, there were no statistical differences in pain scores and the number of dogs that received rescue analgesia among groups.
What Is the Difference Between Rimadyl and Meloxicam?
The two primary differences are that this medication is available as an oral suspension, unlike Rimadyl. In addition, it was the first non-steroidal anti-inflammatory drug the Food and Drug Administration approved for use in cats. But it should be used cautiously in cats under your veterinarian’s supervision.
Which is Stronger, Diclofenac or Meloxicam?
They are equivalent in relieving the acute pain associated with lumbar spine osteoarthritis. However, this drug is much better tolerated.
Is Meloxicam the Same as Ibuprofen?
The main differences between this medication and ibuprofen are: this drug is considered a stronger painkiller than ibuprofen. It is only available on prescription, and ibuprofen is available over the counter and on prescription. It is a long-acting medicine that only needs to be given once.
Is It the Same as Tylenol?
They belong to different drug classes and work differently. So while both NSAIDs and acetaminophen work on the COX enzyme to reduce pain, they differ in how and where they block the enzyme. Nevertheless, they work equally well on pain. However, this drug reduces inflammation, but Tylenol does not.
Can Dogs Take Prednisone and Meloxicam Together?
Mixing this drug with corticosteroids (such as prednisone, prednisolone) or other NSAID drugs is never a good idea. Tell your veterinarian about your pet’s medications (including vitamins, supplements, or herbal therapies).
Can Methocarbamol and Meloxicam be taken together?
No interactions were found between this drug and methocarbamol. However, this does not necessarily mean no interactions exist. Always consult your healthcare provider.
Is This Medication a Narcotic?
No, it is not a narcotic. It is in a non-steroidal anti-inflammatory drug group (NSAIDs). It works by reducing hormones that cause inflammation and pain in the body.
Does It Contain Opioids?
In fact, at one point in time, it gained some attention as a street drug, as people who abused opioids thought that this medication was an opioid. This is not the case. Even though the drug is not an opioid, it has its side effects and risks.
Are There Steroids in This Drug?
Meloxicam is a non-steroidal anti-inflammatory drug (NSAID). It blocks proteins in your body that cause pain and swelling.
Is Meloxicam an Antibiotic?
Meloxicam is not an antibiotic. It is a non-steroidal anti-inflammatory drug (NSAID) used to relieve the symptoms of arthritis (juvenile rheumatoid arthritis, osteoarthritis, and rheumatoid arthritis), such as inflammation, swelling, stiffness, and joint pain.
Is Meloxicam Better Morning or Night?
It does not matter when you give your pet the drug as long as you should give it at about the same time every day. It’s best to give this medication with food to prevent stomach issues.
How Many Times a Day Can I Give My Dog This Medication?
On the first day, the usual dosage is 0.09 milligrams per pound of your dog’s body weight. All subsequent treatments should be administered once a day following the initial therapy. 0.045 milligrams are prescribed for every pound of your body weight.
Do Vets Prescribe Pain Meds After Neutering or Spray?
Dogs, just like people, experience pain following an injury or surgery. Your vet may prescribe a pain-relieving medicine to help make your dog more comfortable at home. You must give the drug according to your vet’s advice to ensure your dog recovers as comfortably as possible. The drug can treat chronic conditions, short-term acute pain symptoms, and inflammation.
Is It Used for Cancer?
In vivo, studies were performed to evaluate the drug’s effect on the growth of HCA-7 cells when xenografted into nude mice. A 51% reduction in tumor size was observed after four weeks of treatment.
Certain oral non-steroidal anti-inflammatory drugs, such as piroxicam (Feldene®) or Meloxicam (Metacam®), have demonstrated anti-cancer activity with TCC and may help some dogs. However, they work best when combined with chemotherapy.
Can the Drug Shrink Tumors?
Treatment with this medication significantly reduced tumor size within three weeks. Please get in touch with your veterinarian for more detailed information.
Can I Give My Dog Meloxicam for Toothache?
It is generally given to control arthritis pain in dogs, although it can be given for many other painful conditions such as injuries, cancer, surgery, dental infections, and more. It is typically given once a day as a pleasantly flavored liquid in dogs.
Can I Give It to Treat Ear Infection in My Dog?
NSAIDs like this drug are safe but ineffective in treating ear infections, although it is a suitable anti-inflammatory medication for dogs.
Does It Reduce Fever?
NSAIDs function by lowering prostaglandin levels, which cause pain, fever, and inflammation. For instance, this medication reduces prostaglandin concentrations by inhibiting cyclo-oxygenase, the enzyme responsible for producing prostaglandins. As a result, temperature, discomfort, and inflammation are diminished.
Can You Give It to Lactating Dog?
The safe use of this medicine in dogs younger than six months of age, dogs used for breeding, or pregnant or lactating dogs has not been evaluated. Therefore, you need to consult your veterinarian to get more information before giving the medicine to your pregnant or lactating dog.


































Do you need a prescription to buy meloxicam on line
Hello! Thank you for contacting us.
As we are a blog we do not sell any drugs. You may use our partner’s website to order Meloxicam online. To do this check the price table at the beginning of the article and follow the link to the website to ask about prescriptions and to order medicines online.